Attrities is a progressive inflammatory condition that affects joints and surrounding tissues, leading to pain, stiffness, swelling, and reduced mobility. It may develop due to genetic factors, immune dysfunction, aging, or long-term wear and tear. Early diagnosis, lifestyle changes, targeted medication, and modern therapies in 2026 significantly improve symptom control and prevent long-term complications when treated promptly.
Attrities is increasingly recognized as a condition influenced by inflammation, immune imbalance, lifestyle habits, and environmental triggers. While symptoms often begin subtly with joint discomfort or stiffness, untreated progression can affect daily activities and long-term mobility. Advances in 2026 treatment approaches now combine early diagnostic imaging, precision medicine, physical rehabilitation, and supportive nutrition plans to control inflammation and restore joint function. Understanding risk factors, recognizing early warning signs, and adopting preventive habits are key to managing this condition effectively and maintaining an active, pain-free life.
What Is This Condition and Why It Matters
Attrities is a chronic inflammatory disorder that primarily targets joints but may also influence surrounding connective tissues. It develops gradually, often starting with mild stiffness or discomfort before progressing into noticeable pain andreduced flexibility. Because joints are essential for movement, untreated inflammation can disrupt everyday tasks such as walking, lifting, or bending. Early awareness is crucial, as timely intervention helps prevent structural joint damage. Medical research continues to highlight the importance of proactive care rather than waiting for symptoms to worsen.
How Inflammation Impacts Joint Health
Inflammation plays a central role in joint deterioration. When the immune system becomes overactive or misdirected, it may attack healthy tissue, leading to swelling and tenderness. Over time, this inflammatory response can damage cartilage, the protective cushioning between bones. As cartilage thins, bones rub against each other, intensifying discomfort. Persistent inflammation also reduces joint lubrication, causing stiffness. Understanding this biological process helps explain why anti-inflammatory treatments and immune-modulating therapies remain central to modern management strategies.
Early Warning Signs You Should Never Ignore
Initial symptoms are often subtle and may include morning stiffness lasting more than thirty minutes, mild swelling, or a warm sensation around joints. Some individuals report fatigue or a general feeling of weakness before noticeable pain begins. Ignoring these early signals can delay diagnosis and increase long-term complications. Tracking symptom patterns and seeking evaluation when discomfort persists beyond a few weeks significantly improves outcomes. Early-stage management is typically more effective and less invasive than late-stage interventions.
Root Causes Behind Joint Degeneration
Multiple factors contribute to joint inflammation and structural damage. Genetics may predispose certain individuals, while autoimmune reactions can trigger abnormal immune responses. Repetitive stress from occupational activities or sports may accelerate wear. Aging naturally reduces cartilage resilience, increasing vulnerability. Environmental influences, including smoking and poor nutrition, further intensify inflammatory responses. Rather than a single cause, the condition often results from a combination of internal susceptibility and external triggers working together over time.
Key Risk Factors to Consider
Certain populations face higher vulnerability, including older adults, individuals with family history of joint disorders, and those with metabolic conditions. Obesity places extra mechanical pressure on weight-bearing joints, worsening inflammation. Sedentary lifestyles weaken supportive muscles, reducing joint stability. Hormonal changes may also influence inflammatory patterns. Identifying personal risk factors allows early preventive measures, including weight management, balanced nutrition, and regular physical activity to maintain joint strength and flexibility.
Modern Diagnostic Approaches in 2026

Diagnosis today relies on a combination of clinical evaluation, imaging, and laboratory testing. Physicians assess swelling, tenderness, and range of motion before recommending advanced imaging like MRI or ultrasound to detect early tissue damage. Blood markers may reveal inflammatory activity or autoimmune involvement. Early detection technologies in 2026 allow healthcare providers to identify subtle structural changes before severe degeneration occurs, enabling more personalized treatment planning and improved long-term outcomes.
Also read this: Fara Cap Complete Guide 2026 – Price, Features & Authentic Details
Latest Medical Treatments Available
Treatment strategies focus on reducing inflammation, relieving pain, and preserving joint structure. Anti-inflammatory medications, disease-modifying drugs, and biologic therapies target immune responses more precisely than older treatments. In some cases, regenerative therapies are explored to stimulate tissue repair. Minimally invasive procedures may be considered if conservative measures fail. Personalized treatment plans now integrate medical therapy with rehabilitation programs, ensuring comprehensive management rather than symptom suppression alone.
The Role of Physical Therapy in Recovery
Structured exercise programs strengthen surrounding muscles, improving joint stability and flexibility. Physical therapists design customized routines that reduce stiffness without overloading affected areas. Gentle stretching, resistance training, and low-impact aerobic activities promote circulation and reduce inflammatory buildup. Consistency is essential, as gradual strengthening enhances resilience. Rehabilitation also teaches posture correction and joint-protection techniques, empowering individuals to manage daily activities with reduced strain and discomfort.
Nutrition Strategies That Support Joint Health
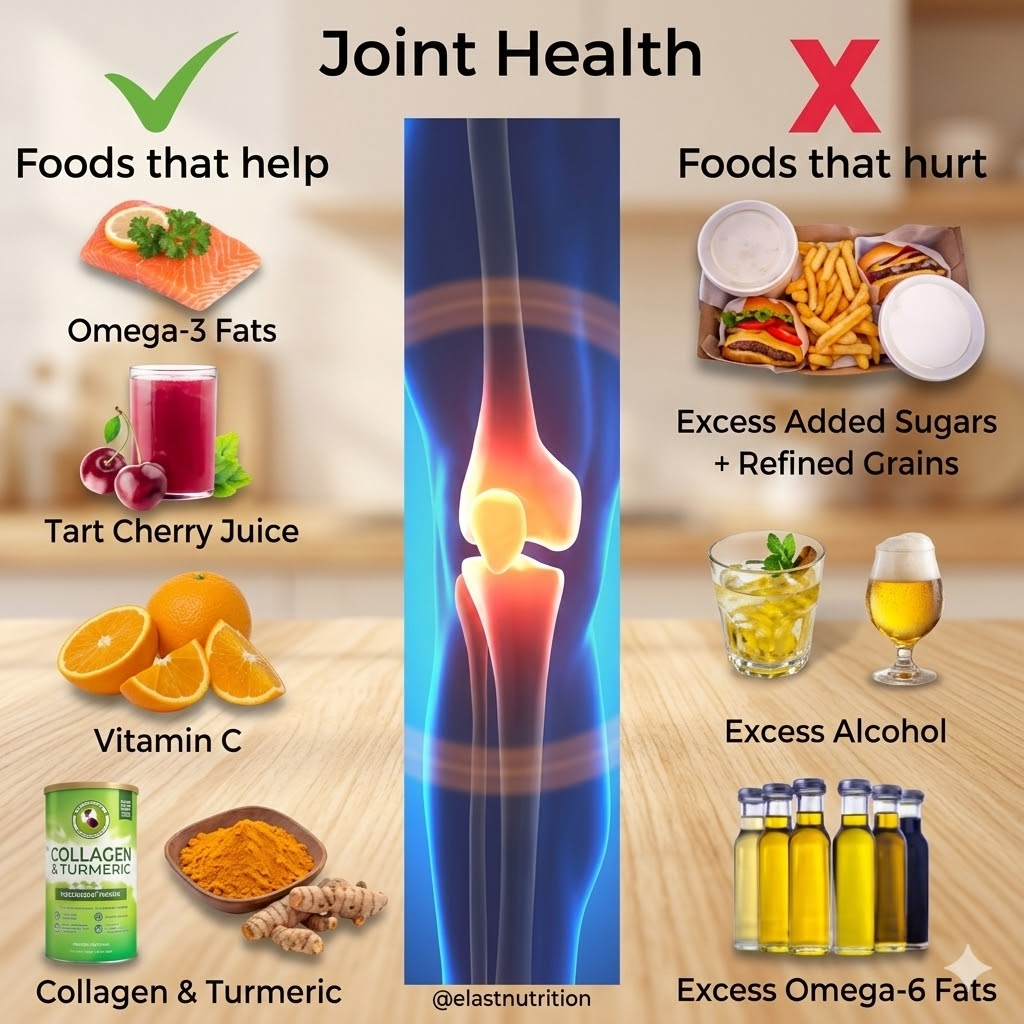
Diet significantly influences inflammatory balance. Omega-3 fatty acids, leafy greens, berries, nuts, and whole grains provide antioxidants that combat oxidative stress. Processed foods high in sugar and trans fats may intensify inflammation. Adequate hydration supports joint lubrication, while maintaining healthy body weight reduces pressure on knees and hips. Balanced nutrition complements medical treatment by supporting immune regulation and tissue repair, making it an integral part of long-term management.
Lifestyle Changes That Improve Long-Term Outcomes
Daily habits greatly influence progression. Regular movement prevents stiffness, while adequate sleep supports tissue recovery. Stress management techniques such as meditation and controlled breathing may reduce inflammatory triggers. Avoiding smoking and limiting alcohol consumption further protects joint health. Small, consistent lifestyle adjustments often produce measurable improvements in mobility and comfort over time, reinforcing the importance of holistic care rather than relying solely on medication.
Potential Complications If Left Untreated
Without proper management, chronic inflammation can lead to joint deformity, persistent pain, and reduced independence. Cartilage breakdown may become irreversible, necessitating surgical intervention. Limited mobility also increases risk of muscle weakness and balance problems. In severe cases, systemic inflammation may affect other organs. Early intervention significantly lowers these risks, highlighting the importance of timely diagnosis and adherence to treatment recommendations.
Preventive Measures for High-Risk Individuals
Prevention begins with maintaining healthy weight and engaging in regular low-impact exercise such as swimming or cycling. Strength training supports joint alignment, while stretching preserves flexibility. Periodic medical check-ups allow early detection of inflammatory markers. Nutritional supplementation, when recommended by professionals, may further protect cartilage health. Preventive strategies are especially important for individuals with family history or prior joint injuries.
Psychological Impact and Coping Strategies
Chronic joint discomfort can influence mental well-being, leading to frustration or anxiety about mobility limitations. Support groups, counseling, and open communication with healthcare providers foster emotional resilience. Maintaining social engagement and hobbies encourages positive outlook. A balanced approach that addresses both physical and psychological aspects contributes to improved overall quality of life and better adherence to treatment plans.
Also read this: Nlpadel: Discover the Hidden Rise of Padel in the Netherland
Surgical Options and When They Are Needed
Surgery is typically reserved for advanced cases where conservative therapy fails. Joint repair, minimally invasive arthroscopy, or total joint replacement may restore function and reduce pain. Advances in surgical techniques improve recovery time and implant durability. However, surgery is considered after thorough evaluation and exploration of non-surgical alternatives. Proper rehabilitation following procedures remains critical for successful long-term outcomes.
Long-Term Outlook and Prognosis
With early detection and modern therapies, many individuals maintain active lifestyles. Continuous monitoring and personalized treatment adjustments prevent flare-ups. Research advancements in 2026 emphasize targeted immune modulation and regenerative medicine, offering hope for improved disease control. Long-term prognosis largely depends on early action, consistent therapy, and lifestyle commitment, underscoring the value of proactive healthcare decisions.
Conclusion
Attrities in 2026 continues to be a growing concern as more people experience its early symptoms due to modern lifestyle factors, environmental triggers, and underlying health conditions. Recognizing the warning signs early—such as persistent discomfort, fatigue, or physical changes—can make a significant difference in preventing the condition from progressing. Early awareness empowers individuals to seek timely medical advice and adopt healthier habits.
Understanding the root causes is equally important. Factors like poor diet, chronic stress, lack of physical activity, and untreated medical issues can all contribute to the development or worsening of attrities. By identifying these triggers, individuals and healthcare professionals can create more targeted and effective treatment strategies.
Fortunately, the most effective treatments in 2026 combine medical innovation with lifestyle-based approaches. Modern therapies, preventive care, balanced nutrition, regular exercise, and proper medical guidance can significantly reduce symptoms and improve quality of life. With the right knowledge and proactive care, managing attrities is not only possible but can also lead to long-term health stability and overall well-being.
FAQs
1. What is the main cause of attrities?
It usually develops due to immune dysfunction, genetic predisposition, aging, and repeated joint stress combined with inflammatory triggers.
2. Can it be cured permanently?
There is no absolute cure, but early treatment and lifestyle management can control symptoms effectively.
3. What are the first symptoms?
Morning stiffness, mild swelling, warmth in joints, and persistent discomfort are common early signs.
4. Is exercise safe?
Yes, low-impact exercise strengthens muscles and reduces stiffness when done under guidance.
5. Which foods reduce inflammation?
Omega-3 rich fish, leafy vegetables, berries, nuts, and whole grains support joint health.
6. When should I see a doctor?
If joint pain lasts more than a few weeks or limits daily movement, medical evaluation is recommended.
7. Are modern 2026 treatments effective?
Yes, advanced biologic therapies and personalized care plans have significantly improved long-term management outcomes.
For more info: voxvison.com